Rosacea usually affects the skin of the face, with episodes of redness, flushing, papules and pustules (pimples), and patches of tiny visible blood vessels (called telangiectasia). It can be very distressing and affect self-esteem and self-confidence. It is considered a chronic condition with variations in intensity and frequency.
It is most commonly diagnosed in women aged 30-50, and usually affects people with fair skin of Northern European ancestry, and women are more often affected than men.
The most common symptom is blushing or flushing, which becomes more persistent and intense over time. Other symptoms become obvious, including pimple-like spots and the telangiectasia described above. The ongoing episodes of flushing lead to inflammation which further irritates the area, giving the appearance of persistent redness.
There are a number of factors involved in the development of rosacea, but an exact cause is still unknown. There is evidence of genetic causes and physical factors (such as vascular and inflammatory), but environmental triggers are considered the most significant factor.
Treatment begins with prevention. For most patients with rosacea, avoiding triggers such as heat, sun exposure, vigorous exercise, emotional stress, hot food and drinks, cosmetics and skin care, sun exposure, and activities that cause flushing, will assist with reducing the most visible symptoms. These triggers may cause or worsen rosacea by dilating blood vessels and sending more blood to the surface of the skin.
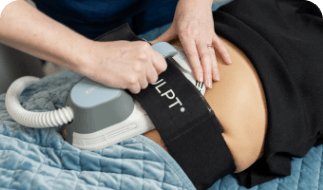
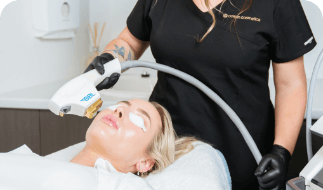
Patients of Ocean Cosmetics are most commonly treated with a combination of regular LED Light Treatments to assist with calming and reducing the redness of the skin as well as a series of BroadBand Light (BBL) treatments every 2-3 weeks to help with the vascular component within the skin.
BBL Photorejuvenation – BBL is a particularly successful and affordable way to treat rosacea. The light based technology triggers the cells regeneration process, so results are visible from the very first treatment.
Light & Laser – Light and laser treatments can be great options for treating rosacea, fine lines and wrinkles, sun damage, pigmentation, age spots and more. Here at Ocean Cosmetic, we have a range of suitable treatments: BBL, BBL Hero, Healite LED, MOXI, Clear + Brilliant, Fraxel and Revlite Q Switch.
We recommend coming in for a consultation to see what treatment option is the best for you.
Recommended treatments

Dr Gina
“Unfortunately rosacea can’t be cured, but it can be treated and managed with holistic treatment plan. As always, your skin should be protected from the sun with spf, try to avoid triggers, and visit the clinic for a treatment plan. Laser and light based treatments have been an effective way to reduce the redness caused by rosacea.”
DR GINA MESSIHA
(Cosmetic Doctor) MB BS FRACGP